With Cigna’s recent announcement that it intends to purchase Express Scripts, five of America’s top health insurance companies now own or plan to own pharmacy benefit managers (PBMs).
The move is the latest example of vertical integration in the health insurance industry. This pattern continues at a time when PBMs are receiving intense scrutiny regarding their candidness and effectiveness in lowering drug costs.
Which other big-name companies are bringing PBMs into their fold, and why are they doing it? As Aetna CEO Mark Bertolini said in his 2017 Q1 earnings call, it seems “going forward, the PBM relationship as a standalone model is a troubled relationship.” Let’s explore why.
Listen to this article:
A Trend in the Making
As recently as 2017, the three largest PBMs operated by completely different business models: Express Scripts remained independent, OptumRx was owned by an insurance company, and CVS Caremark was run by pharmacy chain CVS Health. Now, they could all soon be under the control of nationwide insurers.
Back in 2015, we saw UnitedHealth Group’s OptumRx purchase then fourth-largest PBM, CatamaranRx. We also saw Aetna announce its intention to acquire Humana; a deal which the Department of Justice blocked a year and a half later after their antitrust review. The failed acquisition would have brought Humana’s PBM services in-house for Aetna.
In October 2017, Anthem announced that it would not renew its contract with Express Scripts, but instead, launch its own PBM, IngenioRx, in 2020. More recently, Aetna also made clearer its intention to control a PBM with its December 2017 proposal to merge with CVS Health in a $69 billion deal. And just last month, Cigna divulged its agreement to purchase Express Scripts for $52 billion.
Five Top Nationwide Insurers and Their PBM Partners
| Insurers | PBM Partners |
|---|---|
| UnitedHealth Group | OptumRx (in-house); CatamaranRx (purchased 2015) |
| Anthem | IngenioRx (launching in-house in 2020) |
| Aetna | CVS/Caremark (purchase under review) |
| Cigna | Cigna Pharmacy Management (in-house); Express Scripts (purchase under review) |
| Humana | Humana Pharmacy Solutions (in-house) |
Clearly insurance companies have an interest in reining in control of PBM operations, but why the acquisitions and consolidation?
The Appeal of the PBM
PBMs, which arose in the 1960s, are “middlemen” designed to process the substantial number of “small-dollar” prescription drug claims for insurance companies and plan sponsors. They use their large purchasing power to negotiate prices with pharmaceutical manufacturers and impact almost every aspect of the prescription drug marketplace.
How did they grow to play such a significant role in health care? As coverage expanded with the inception of the Medicare Part D program in 2006 and the Affordable Care Act in 2010, insurers became more interested in outsourcing management of prescription claims and client services. PBMs stepped in to lighten the load.
Today, PBMs handle far more than claims processing, including drug utilization review, drug plan formulary development, determining which pharmacies are included in a prescription drug plan’s network, deciding how much network pharmacies will be reimbursed for their services, and operating mail order and specialty pharmacies themselves. With drug prices continuing to rise, companies, lawmakers, and other individuals are questioning if PBMs have been abusing their power and pocketing large savings from pharma manufacturer rebates that, in theory, could be passed down to consumers.
A major reason why Anthem will allow its contract with Express Scripts to end at the close of 2019 is it believes Express Scripts withheld billions in savings and overcharged them for services. Modern Healthcare reports PBMs have been criticized for keeping their rebate deals with drugmakers guarded by nondisclosure agreements.
According to insurers, employers want drug pricing to be more transparent. With more oversight of PBMs, insurers could provide their clients with this increased transparency and streamline and further integrate their members’ care. In turn, this could lead to lower prescription drug costs for consumers — but there’s a good chance it won’t.
If drug manufacturer rebates become more transparent, the drug manufacturers themselves could then use information about their competitors to minimize their rebate amounts. This would make drug manufacturers more competitive, which would lead the overall price of drugs to go up, not down. Moreover, for the average joe to see lower prescription drug prices from these mergers, insurers would have to pass on the rebate savings they negotiate to beneficiaries. Right now, it’s likely companies are more interested in claiming a “rich” slice of the pie before it’s gone.
Market Share
Due to their expanding involvement in the prescription drug industry, PBMs pull in profits from several different directions. Industry experts surmise that, as baby boomers age, health care and prescription drug spending will continue to rise, meaning more revenue for these claims processing giants.
According to a 2015 Applied Policy report, the top three PBMs in the country manage the drug benefits of 78% of the U.S. population, or 180 million people. Pending the approval of the Aetna-Caremark and Cigna-Express Scripts deals, these giants would be linked to three colossal insurers.
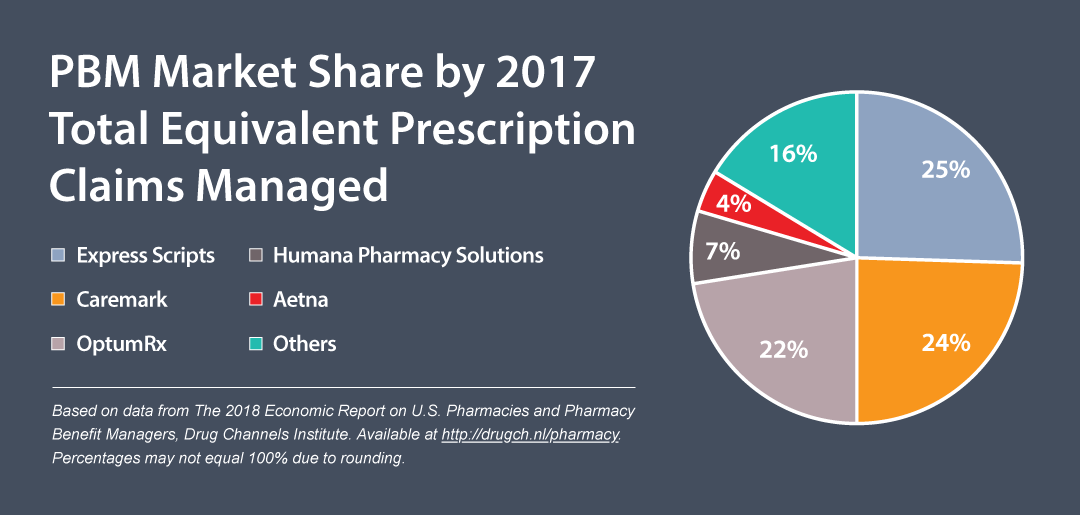
When looking at prescription claims managed, OptumRx (22%), Caremark (24%), and Express Scripts (25%) dominated the market in 2017. The pending mergers could propel Cigna and Aetna to surpass UnitedHealthcare in PBM market share, providing the number of claims processed by each of the companies remains about the same in the future.
As for Humana, at the end of March, The Wall Street Journal reported that massive retailer Walmart Inc. is “in preliminary talks” to purchase the insurer. Such a deal would be similar in nature to CVS Health’s acquisition of Aetna, Rite Aid Corp’s 2015 acquisition of PBM EnvisionRx Plus, and Albertsons Cos. proposed acquisition of Rite Aid Corp.
Humana and Walmart already have a co-branded drug plan together, so it wouldn’t be a surprise if they chose to further their existing partnership. Creating a stronger bond with Walmart could get Humana more customers. Additionally, combining with Humana would give Walmart another way to stay competitive with Amazon. Speculation that the online retail behemoth will expand into prescription drug sales may have influenced many of the health care related merger proposals we’re seeing today.
Looking to the Future
The CVS-Aetna, Cigna-Express Scripts, Albertsons-Rite Aid, and potential Walmart-Humana mergers will all need to be reviewed and approved by the Antitrust Division of the Department of Justice for them to go through. If they do, insurers should have more control over drug pricing, but it’s not clear as to whether shoppers will see decreased provider options or increased savings from insurers.
In early March, UnitedHealthcare committed to passing rebate savings on drugs to its fully insured group health members on an individual basis at the point of sale beginning in 2019. Aetna has also said it will pass negotiated drug discounts on to about three million of its members next year. Others could follow suit, but that’s anybody’s guess.
Lawmakers in the federal and state governments are also examining PBMs and introducing regulation attempting to reform some of their more questionable practices.






Share Post